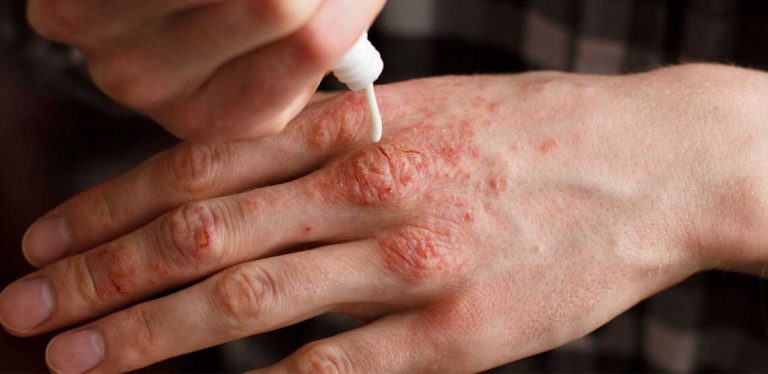
Palmoplantar Psoriasis
Palmoplantar psoriasis is a variant of psoriasis that specifically affects the palms of the hands and the soles of the feet. Psoriasis is a chronic inflammatory condition characterized by scaly, red, thickened areas of skin, referred to as plaques. While psoriasis can occur anywhere on the body, palmoplantar psoriasis is confined to the hands and feet. Palmoplantar psoriasis is responsible for 3% to 4% of all psoriasis cases and can affect patients of any age.
What Are the Causes of Palmoplantar Psoriasis?
As a variant of psoriasis, palmoplantar psoriasis is an autoimmune condition. It develops when the immune system malfunctions, causing new skin cells to produce more quickly than needed. Excess skin cells then accumulate on the surface of the skin, forming the characteristic plaques. While the exact cause of palmoplantar psoriasis is unknown, it is thought that a combination of genetic and environmental factors is involved.
Signs and Symptoms
Common signs and symptoms of palmoplantar psoriasis include:
- Areas of scaly, red, and thickened skin (these areas are typically well-defined)
- Itching or burning
- Cracking
- Bleeding
- Pain or discomfort
What Are the Risk Factors?
Individuals are more likely to be diagnosed with palmoplantar psoriasis if they have family members with the condition. However, while genetics is thought to play a key role in the development of psoriasis, lifestyle choices and environmental triggers may also have an impact. An external factor may trigger the development of palmoplantar psoriasis in an individual who has a family history of the disease. The hands and feet are readily exposed to chemical and environmental triggers. Smoking, irritation, exposure to allergens, and trauma or injury may all act as triggers for the condition. A key preventable risk factor is stress, which affects the functioning of your immune system.
Those with other autoimmune conditions, such as type 1 diabetes, thyroid disease, or celiac disease, also have a greater risk of being diagnosed with palmoplantar psoriasis.
Treatments Options
Like other variants of psoriasis, this type cannot be cured, so the aim of treatment is symptom management. The majority of psoriasis treatments work by slowing down the rate at which affected skin cells grow, helping to reduce inflammation.
The treatment options for palmoplantar psoriasis are the same as those offered to patients with classic plaque psoriasis. As the skin on the palms and soles is thicker, palmoplantar psoriasis may be harder to treat. To relieve the troubling symptoms, patients may be offered the following therapies (either alone or in combination):
Related Search Topics (Ads)
Topical Treatments
- Topical steroids: These are commonly used to treat psoriasis by slowing down skin cell growth, reducing inflammation, and relieving itching.
- Topical emollients: These can help to moisturize and soften the skin, reducing irritation and inflammation.
- Topical retinoids: Derived from vitamin A, they help by slowing down skin cell growth. Retinoid treatments can sometimes cause the skin to become dry and irritated.
- Coal tar: This is one of the oldest known psoriasis treatments. In the form of creams, ointments, or gels, coal tar products provide an inexpensive yet effective treatment for palmoplantar psoriasis. As this treatment can be messy, it is often advised to apply the product at nighttime under cotton socks or gloves.
- Keratolytic agents: These include urea, lactic acid, and salicylic acid. They help to reduce the thickness of scaly plaques by causing the outer layer of skin to break down and shed.
Artificial Light Therapy
More severe cases may require artificial light therapy. This may involve narrowband UVB (NB-UVB) or photochemotherapy (PUVA) (a treatment combining oral or topical psoralen with long-wave UVA).
Oral Treatments
Oral medications are only usually prescribed in severe cases of palmoplantar psoriasis. Effective oral therapies include methotrexate, cyclosporine, and retinoids. Immune-altering biologic therapies are generally reserved to treat more difficult cases where patients have failed to respond to other oral and topical agents.
How to Manage It
There is no denying that psoriasis can be a painful and debilitating condition that, left untreated, can seriously impact your quality of life. Luckily, there are many things that you can do at home, in conjunction with the medications prescribed by your doctor, to help manage your symptoms.
Helpful lifestyle changes include:
- Use mild cleansing agents and take a daily bath using a mild bath oil
- Regularly use a gentle moisturizer
- Stop smoking and limit stress and alcohol consumption
- Protect your feet by wearing comfortable and well-fitting shoes
- Avoid injuries and friction
- Follow a healthy diet and make sure to stick to a gluten-free diet if you have celiac disease
- Maintain a healthy weight
- Avoid getting too much or too little sunlight